Key messages
- Current HTA processes often adopt a narrow healthcare payer perspective, focusing on direct system costs and patient outcomes. While this simplifies decision-making and reduces uncertainty, it systematically excludes indirect costs and spillover effects on carers, families, and society.
- Adopting a broader perspective on value, especially in conditions with clear spillover effects such as breast cancer, can better capture the full societal impact of disease and treatment, ensuring decisions target improved overall wellbeing, not just reduced costs for healthcare systems.
- While broader perspectives introduce challenges, such as data gaps and increased decision uncertainty, we recommend their routine adoption in cases with significant spillover effects. This targeted approach balances ambition with feasibility and incentivises data collection to reduce uncertainty over time.
This Contract Research Report was commissioned and funded by AstraZeneca and Daiichi Sankyo and was developed by the Office of Health Economics (OHE).
In this Whitepaper, we describe different perspectives that can be adopted in Health Technology Assessment (HTA), and some of the advantages and disadvantages of these different perspectives. Drawing a panel session at the 2024 European meeting of the International Society for Pharmacoeconomics and Outcomes Research (ISPOR), including patient, clinical, and health economics representatives, we argue for a broader perspective on costs and outcomes when assessing the value of new treatments, especially when a health condition or its treatment has significant health or economic impacts beyond the patient.
In the context of Health Technology Assessment (HTA), perspective refers to the ‘point of view’ or ‘scope of concern’ adopted when weighing outcomes and costs in an economic evaluation (Drummond et al., 2015). Several perspectives are recognised in HTA, and the appropriate perspective will depend on the context and objectives of an assessment (Sittimart et al., 2024):
- Healthcare Payer Perspective: This narrow view focuses on direct costs to the healthcare system and patient outcomes, such as diagnosis, treatment, and hospitalisation costs. It is commonly used in publicly funded systems with strict budget constraints. This perspective simplifies evaluations and maximises potential health gains under a fixed budget, known as technical efficiency.
- Healthcare Sector Perspective: A slightly broader view that includes direct (out-of-pocket) medical costs to the patient.
- Societal Perspective: This perspective expands the scope of concern to consider all health or direct and indirect economic effects related to a patient’s illness. It may include indirect costs to the patient (lost productivity, leisure time), costs and health impacts to carers and family, and non-health impacts on sectors like education and justice. This perspective aligns with welfare economics in aiming to maximise societal welfare, known as allocative efficiency.
Overview of (especially cost) considerations by perspective
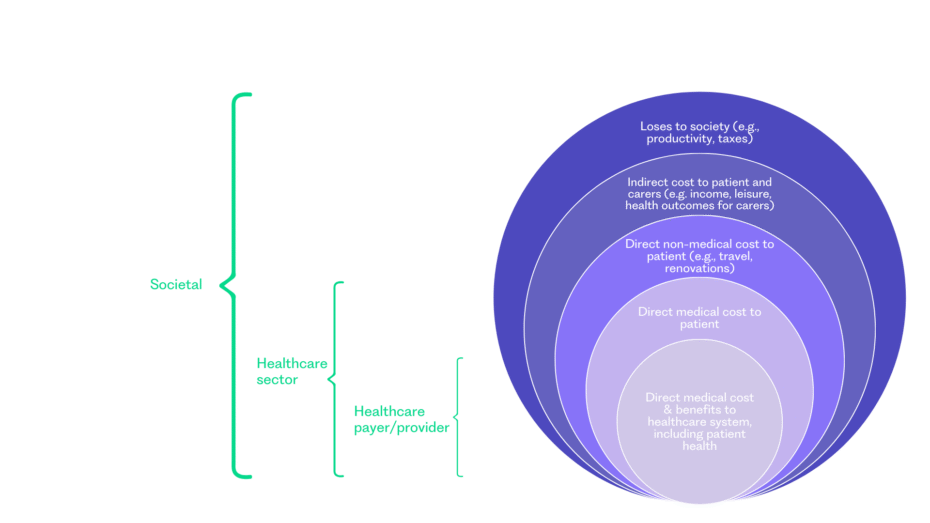
Many health conditions have direct or indirect impacts beyond the healthcare system and can affect more than just the patient and the healthcare system. Indirect costs, not directly related to treatment, include monetary losses to the patient from time off work, or forgone education and leisure. Equally, “spillover effects” impact individuals beyond the patient, such as monetary and health impacts on carers, family, or the wider society (Basu and Meltzer, 2005; Wittenberg, James and Prosser, 2019; Mendoza-Jiménez, van Exel and Brouwer, 2024). The concept of spillover effects could even extend to consideration of ‘unrelated healthcare costs’ in HTA (Kearns, 2020). Depending on the perspective adopted, these indirect costs and spillover effects may or may not be considered in an HTA.
Given potentially important indirect costs and spillover effects, adopting an appropriate perspective is crucial for understanding the full impact of a disease and the value of its treatment. Systematically excluding indirect or spillover costs and health impacts can lead to suboptimal HTA recommendations. For example, early hospital discharge may seem cost-saving from a narrow payer perspective, but a broader view would consider the costs and health effects of shifting care to individuals outside the healthcare system. At the extreme, by disregarding potentially important impacts beyond the patient and the healthcare system, narrower perspectives on value have the potential to improve health outcomes to the patient or save costs for the system but ultimately reduce overall societal welfare in terms of wider costs and burdens (Brouwer, 2019a). Conversely, adopting a broader perspective on value is more likely to ensure recommendations lead to overall societal welfare gains, particularly in cases where conditions or their treatments have clear spillover effects.
Concerns around a broader perspective in HTA may be overstated
Concerns have been raised around the feasibility or appropriateness of broader perspectives on value in HTA, but we suggest that these may be overstated or otherwise manageable:
| CONCERN | RESPONSE |
| The primary objective of healthcare should be to produce (patient) health, not societal welfare. | An overly-narrow focus can mean that health gains to a patient come at the expense of unrecognised and unaccounted losses to others. |
| Including broader impacts requires additional effort to collect and analyse. As these impacts become increasingly removed from the patient or the health system, the uncertainty in these estimates increases. | Defining the scope of an evaluation based on effort rather than relevance is difficult to justify on a theoretical or practical level. HTA bodies may justifiably object that there is limited or uncertain data for broader value elements, but study sponsors may justifiably argue that they have little incentive to invest in the collection of such data until HTA bodies confirm their willingness to adopt a broader perspective in their appraisals. |
| Incorporating broader value elements will increase value-based prices or otherwise threaten the financial sustainability of health systems. | Where a new health technology provides a marginal gain in societal welfare, impact on a value-based price will be correspondingly marginal. However, in cases where a technology does provide a substantial improvement in societal welfare, these gains should be appropriately reflected in value assessment. We note, however, that adopting a different perspective on value will also likely require HTA bodies to adopt a different value threshold. |
| Valuing people’s time would disadvantage unemployed or (typically older) retired individuals and those engaged in lower-paid or volunteer activities, leading to equity concerns. Considering the monetary value of time gained or lost could lead to double-counting if people also consider time away from their usual activities as part of the health-related quality-of-life of a health state. | It would be straightforward to assign a single, representative value of time to all individuals, regardless of their income or employment status. A representative value of time would be consistent with valuing all individuals’ ability to make choices about how they use their time, regardless of the activity. Empirical studies have consistently demonstrated that individuals do not consider time or income losses in their utility valuations, suggesting concern for double counting may be unwarranted, or at worst, minor. |
| A genuine societal perspective on welfare requires some transferability of resources between sectoral budgets as new opportunities to generate societal welfare arise, but such transferability is difficult or impossible under the current system of siloed budgets. | Adopting a broader perspective on value within healthcare would still be a step towards greater allocative efficiency and improved overall societal welfare, and transferability between healthcare budgets may be more achievable in the shorter term. |
A pragmatic way forward: a broader perspective in the presence of spillover effects
We believe a broader perspective on value can lead to better societal outcomes than narrower perspectives, by allowing decision-makers to balance the burdens and benefits to everyone, not just the patient. However, we also understand that methods and interpretations are rapidly developing. For now, we suggest adopting a broader perspective in cases where there are clear spillover effects associated with a disease or its treatment. In these cases, an appropriately broad perspective is necessary to account for the full range of impacts beyond the patient and the healthcare system.
Breast cancer is one such example of a condition with clear spillover effects. As discussed in the ISPOR panel session, breast cancer is associated with substantial costs and burdens extending beyond the patient and the healthcare system. A 2018 analysis of chemotherapy for early-stage breast cancer in the UK found that costs to patients, carers, and wider society were 40% greater than direct treatment costs.
A survivor’s account given at an Educational symposium at the 2024 ISPOR Europe conference also highlighted burdens of breast cancer and its treatment that would not be recognised within the narrow payer perspective. These include the need for support from paid or unpaid (informal) carers during treatment, the need for special diets, prosthetics, and clothing during and after treatment, and long-term effects that can impair survivors’ ability to return to work or make full use of their time.
We note that a limitation of this pragmatic approach is the need to define what constitutes “clear” spillover effects, and to appropriately estimate their costs. Any such definition will be intrinsically subjective, and it may be difficult to be consistent in the consideration of financial spillovers and more humanistic spillovers. Arguably, this supports routine adoption of a broader perspective, but in the shorter-term we suggest that continuing research on a ‘multiplier’ for relative spillover effects by condition may help to inform when spillover effects are likely to be more relevant to an HTA decision.
Conclusion
A narrow perspective on value simplifies the HTA process and may reduce decision uncertainty, but it excludes potentially important impacts on patients, carers, family members and wider society, and may lead to situations where HTA maximises health at the expense of broader societal welfare. A broader perspective on value may add some decision uncertainty but can better support decisions that can improve overall societal welfare beyond patient health.
In recognition of some of the challenges associated with broader perspectives on value, particularly the potential for greater decision uncertainty (at least in the short term), we recommend that HTA bodies routinely adopt a broader perspective on value in circumstances where there are recognised spillover effects associated with a condition and its treatment. As we have demonstrated here, including through the first-hand account of a survivor, this category includes breast cancer.





