For the growing number of multi-indication medicines, access may be delayed or even denied due to challenges in linking payment with a medicine’s value across those…
For the growing number of multi-indication medicines, access may be delayed or even denied due to challenges in linking payment with a medicine’s value across those indications. We assembled a broad range of stakeholders to work toward consensus on the challenges and solutions which promote better patient access and sustainable health care and innovation.
Traditionally, medicines are priced per pill or vial, with the price determined or anchored in some way to value (benefits for patients and value-for-money). However, individual medicines are increasingly found to benefit patients in a range of indications, within or across diseases, at different stages of disease, as monotherapy or in combination with other therapies as part of treatment regimens. The “value” of these multi-indication medicines is likely to vary substantially between indications, which challenges our single-price paradigm.
Science is out of step with payment models and it’s time to ask: What should payment models for pharmaceuticals aim to achieve, are they being achieved for multi-indication medicines, and can we do better?
To find the best solutions we must balance many perspectives. First and foremost, patients (and their treating clinicians) want access to the most effective treatments. Payers have accountability for enabling access within the context of the resources and treatment options that are available today. Health care systems more broadly strive to make effective and affordable treatments available and to foster an environment that incentivises the development of those treatments. Those responsible for discovering, developing and bringing innovation to market are motivated by advancing patient care while maintaining a sustainable business model. In order to overcome challenges in the pricing and reimbursement of medicines, we need to take all of these perspectives into consideration.
Between April and May 2021, OHE convened 16 experts from 11 countries, with perspectives covering the patient, payer, health technology assessment decision-maker, policymaker, health care provider/clinician, regulator, data expert, health economist and industry. Through a pre-meeting survey, virtual meeting and two-week online platform meeting, we used a modified Delphi approach to work toward consensus on the principles of the problem and solutions for multi-indication therapies, complemented by a payer survey and supplementary research to address the evidence gaps.
This report summarises that research, which was commissioned and funded by AstraZeneca, and the main conclusions of the expert consensus programme are summarised in the Figure below.
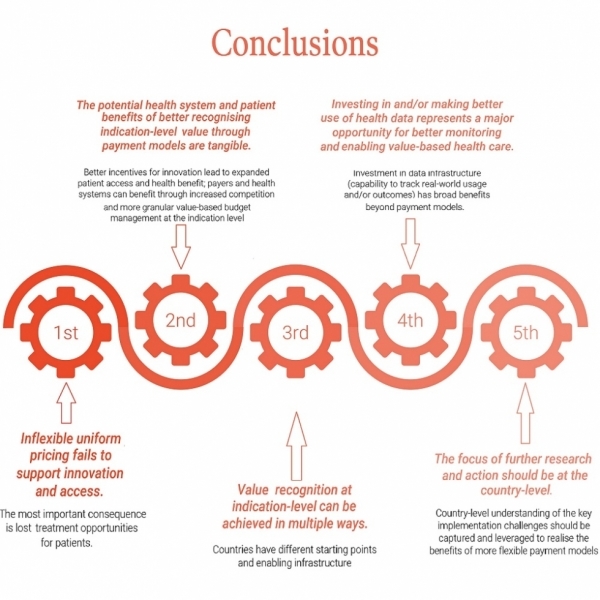
Through the research, we have – along with an international panel of experts – been on a journey to better understand the need for and opportunities associated with payment models that recognise value at the indication-level, as well as the challenges associated with their implementation and how they can be overcome.
The expert panel considered that the main objectives of pricing that are not well addressed by inflexible uniform prices are: optimising incentives for innovation and optimising access for patients, and that differentiating payment based on value at the indication-level represents an important part of the solution for multi-indication therapies. Value recognition at indication-level can be achieved in multiple ways, including blended pricing (with actual/estimated usage), single price with differential adjustments, and outcome-based payments. The evolution of medical innovation and the need for sustainable financing requires health systems to adapt their payment models in ways that value clinical benefits in ever-smaller and multiple patient groups. Data systems must be utilised and evolve to accommodate this need, in order to realise full benefits of medical innovation for patients and health systems.
Citation
Cole, A., Neri, M. and Cookson, G., 2021. Expert Consensus Programme: Payment Models for Multi-Indication Therapies. OHE Consulting Report, London: Office of Health Economics. Available at: https://www.ohe.org/publications/payment-models-multi-indication-therapies
See here for the report appendices.
Related Research
Cole, A., Towse, A., Lorgelly, P., and Sullivan, R. (2018) Economics of Innovative Payment Models Compared with Single Pricing of Pharmaceuticals. OHE Research Paper. Available from https://www.ohe.org/publications/economics-innovative-payment-models-compared-single-pricing-pharmaceuticals-0.
Cole, A., Towse, A., Zamora, B. (2020) Indication-Based Pricing (IBP) Consultation Report. OHE Consulting Report. Available from https://www.ohe.org/publications/indication-based-pricing-ibp-consultation-report.
Neri, M., Towse, A. and Garau, M., 2018. Multi-Indication Pricing (MIP): Practical Solutions and Steps to Move Forward. OHE Briefing. Available from https://www.ohe.org/publications/multi-indication-pricing-mip-practical-solutions-and-steps-move-forward.
Towse, A., Cole, A., and Zamora, B. (2018) The Debate on Indication-Based Pricing in the U.S. and Five Major European Countries. OHE Consulting Report. Available from https://www.ohe.org/publications/debate-indication-based-pricing-us-and-five-major-european-countries.