Obesity is an increasing challenge in England, as elsewhere. OHE has completed a study that examines PCT practice and the cost savings that could accrue if…
Obesity is an increasing challenge in England, as elsewhere. OHE has completed a study that examines PCT practice and the cost savings that could accrue if NICE guidance was followed more closely.
Obesity is an increasing problem in England, as it is in many countries worldwide. In 2008, nearly a quarter of adults aged 16 and over were classified as obese, according to an NHS report, up from about 15% in 1993. This is expected to double by 2050 unless effective action is taken. The impact on NHS costs for treatment of illnesses related to obesity is substantial, with the Department of Health estimating the costs at £4.3bn per year.
In December 2006, the National Institute for Health and Clinical Excellence (NICE) issued guidelines for preventing and managing overweight and obesity. Recommendations are step-wise, starting with lifestyle changes and progressing through medicine to bariatric surgery. The guidance recommends that patients considered for bariatric surgery have either a BMI of 40 or more or a BMI over 35 with an associated condition such as diabetes. Costing guidelines are included in the guidance.
OHE has just published the results of a study that examines current provision of bariatric surgery in England and estimates the cost savings that would be produced if if NICE guidance was followed closely. The project included surveying PCTs about current practice, a literature review of the indirect costs of obesity, and the development of a model that combines the NICE costing guidelines with other costs and benefits identified in the literature.
PCTs were asked to assess whether they follow NICE guidelines for obesity. Nearly 40% reported their referral guidelines were in line with them in all respects; nearly 50% stated that elements of their guidelines match elements of the NICE guidelines; about 10% stated they do not follow the guidelines at all. Official statistics suggest that PCTs either do not follow the NICE guidelines or are interpreting them stringently. The economic model developed as part of this project estimates that approximately 11,000 to 140,000 people in England currently qualify for bariatric surgery under NICE guidelines. The actual number of surgeries that took place in England in 2009-10 was 3,607. Thus, adherence is generally sub-optimal. Wide variation among PCTs also exists: the number of procedures commissioned by the 151 PCTs who commission care for local populations in England ranged from 1 to 192 in 2009-10.
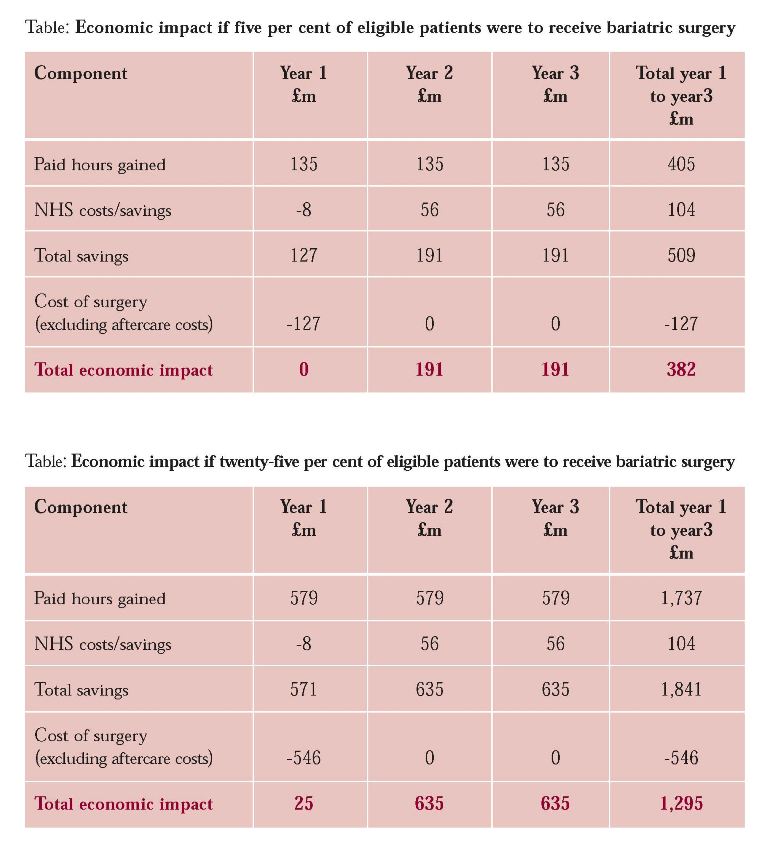
The OHE's economic model found that the contribution of additional paid work following bariatric surgery off-set the costs of surgery one year after surgery. Further savings also accrue from reductions in welfare benefits paid and, although the evidence base is limited, savings for the health service. The two tables below detail costs and savings estimated in the report. (These tables do not include what would be saved from reductions in welfare benefits payments, which are between £35m and £150m per year.)
(click on table for larger image)
Results from the PCT survey indicate that one-third of PCTs expected to apply the NICE guidance more stringently in future and none was planning to apply the guidelines less stringently.
Download O'Neill, P. (2010) Shedding the pounds: Obesity management, NICE guidance and bariatric surgery in England. London: Office of Health Economics.